Should everyone wear medical masks to prevent the spread of COVID-19?
Types of medical masks
A. Surgical masks versus respirators
Well before the COVID-19 pandemic, there was evidence from health care settings that medical masks—which include surgical masks (also called medical or procedure masks) and respirators—protect health care workers from respiratory infections. There are important differences between surgical masks and respirators. The filters of both surgical masks and respirators are made from mats of fine fibers, and differences in fiber diameter, density and filter thickness affect how well a mask collects particles. Filters do not simply function as sieves; rather, filters collect and trap particles over a range of sizes. Some filters are constructed from charged fibers, and electrostatic attraction can increase the collection of both larger and smaller particles. To be certified for use in health care settings in the U.S., the performance parameters for surgical masks are less stringent than those for respirators. Surgical masks are also looser fitting than respirators and do not prevent air from leaking between the mask and the face.
When a person exhales, talks, sings, coughs, or sneezes, they release respiratory droplets into the environment. If the person is infected with a respiratory virus, the droplets they exhale may contain the virus. Surgical masks can protect wearers from exposure to droplets and prevent the release of infectious respiratory droplets into the environment. People exhale both larger droplets that do not travel far before they fall out of the air and tiny particulate droplets that can remain suspended in the air and travel a longer distance. The public health and medical community has traditionally referred to transmission by tiny particles as “airborne transmission.” There are two aspects of airborne transmission, and they are sometimes confused. The first is the size of the droplet: large or small. The second is the distance between the source of infection and the person at-risk of infection. It is likely that SARS-CoV-2, the virus that causes COVID-19, may be transmitted within a range of droplet sizes including small particles, but transmission occurs mostly in close quarters—about 6 feet or less. When a patient is suspected or confirmed to have a disease that may be spread by airborne transmission, it is recommended that health care workers wear respirators to protect themselves from infection.
B. Types of respirators
A respirator is a device that covers at least the nose and mouth and reduces the wearer’s risk of inhaling invisible small particles including gases, dust and infectious agents carried on tiny respiratory droplets. In the U.S., respirators are certified for use in health care settings by the National Institute for Occupational Safety and Health (NIOSH), a branch of the U.S. Centers for Disease Control and Prevention (CDC). During the certification process, respirators are tested to make sure that their filters capture a range of hazardous particles of many sizes over a range of airflows. A common type of respirator is the disposable filtering facepiece respirator (FFR). The most common type of FFR used in the U.S. is an N95 respirator, which is designed to filter out 95% of tiny particles. There are many brands of NIOSH-certified N95s. In addition to FFRs, there are elastomeric respirators, which are reusable respirators made of synthetic material or rubber, and powered air purifying respirators, which are reusable battery-powered devices that suck in air through filters.
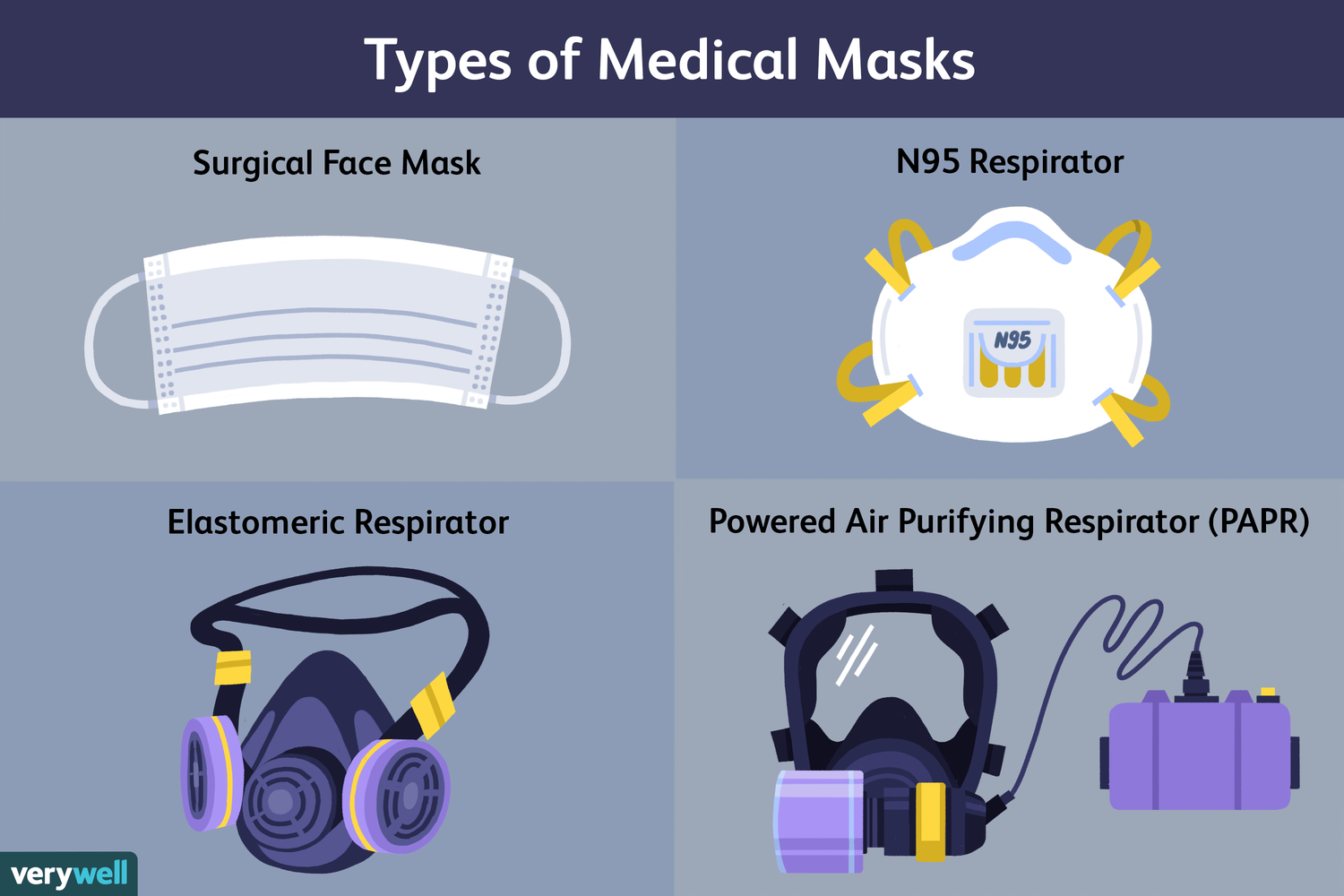
Source: Very Well Health
Filtering facepiece respirators designed to have similar filter efficiencies as the N95 respirator are certified by international regulatory agencies using alternative classification schemes. These FFRs include the KN95 (China), KF94 (South Korea) and FFP2 (Europe). To increase the availability of FFRs to the U.S. health care workforce during the COVID-19 pandemic, some of these products have been granted authorization for emergency use by the FDA. It is important to note that the quality of the filter alone does not guarantee protection; protection also depends on the fit of the FFR to the wearer’s face. For an N95 to successfully filter out 95% of particles, there should be a good seal between the respirator and face so that particles don’t leak through a gap and escape the filter. For example, people with beards cannot usually achieve a good protective seal with N95s, and KN95s may not fit users’ faces as well as N95s. The Occupational Health and Safety Administration stipulates that health care workers who need respiratory protection should undergo fit testing and training each time they use a respirator they haven’t used before, and yearly thereafter. It is also recommended that each FFR user perform their own seal-check with each use, but there is evidence that self-assessments correlate poorly with the results of formal fit testing. This highlights the importance of standardized assessment and user training for FFRs to be maximally protective.
The role of respirators in preventing the spread of COVID-19: maximum protection for the wearer
Evidence suggests that most transmission of SARS-CoV-2 occurs via droplets dispersed over shorter distances. However, reports of SARS-CoV-2 transmission on buses, during choir practice, and in nursing homes with poor ventilation suggest that airborne transmission over longer distances can also occur. The chance of transmission increases with poor ventilation; exposure to numerous contacts; longer durations of exposure to contacts; and activities that may generate infectious droplets and particles, including speaking, coughing and medical procedures such as intubation. For these reasons the CDC recommends that health care workers wear respirators to protect themselves from infection when caring for patients known or suspected to have COVID-19, or when intubating a patient who could have COVID-19. It is well established that health care workers with patient-facing roles are at increased risk of COVID-19 compared to the general population. In health care and other high risk settings, maximum respiratory protection for the mask wearer is a priority.
Evidence supports that filtering facepiece respirators (FFRs) help protect health care workers from COVID-19. Studies have shown that mask use reduces the risk of COVID-19 among health care workers. A review of risk factors for coronavirus infections among health care workers found that the factor most consistently associated with reduced risk of COVID-19 was the use of personal protective equipment; mask use had a stronger relationship with decreased risk of infection than any other protective measure. There is some evidence that surgical masks and N95s offer health care workers similar protection, whereas other studies suggest that N95s lower the risk of COVID-19 when compared with surgical masks. For example, in one study of 1,818 health care workers who reported exposures to COVID-19, the prevalence of antibodies to SARS-CoV-2 was significantly lower among those who wore respirators (10%) than among those who wore surgical or other masks (13%) or no masks (18%). There is little evidence on the protection cloth masks may offer health care workers. Pre-pandemic evidence suggested that health care workers who wore cloth masks were less protected against influenza than health care workers who wore other types of masks.
The role of non-respirator masks in preventing the spread of COVID-19: source control and protection for the wearer
At the beginning of the pandemic, there were questions about whether to use masks in the community and the appropriate role for filtering facepiece respirators (FFRs). There were concerns that FFRs might not offer strong protection if they were reused, if users were not trained how to wear them, or if they were not properly fit tested. However, such questions on FFR effectiveness outside health care settings were rendered moot by the fact that not even health care workers had sufficient access to FFRs. Over the past year, our understanding of SARS-CoV-2 transmission, the role of masks in reducing transmission and the effectiveness of non-medical masks in reducing transmission has evolved. Currently, both U.S. and international public health authorities recommend the use of non-medical masks in the community, supported by several strong lines of evidence:
1) Mechanistic evidence that non-medical masks can efficiently filter droplets:
Numerous mechanistic studies have shown that cloth masks can efficiently filter droplets across a range of sizes and airflows and that some cloth masks filter droplets as well as some surgical masks. The extent of filtration has been found to vary significantly by material type. For example, one study that assessed the filtration efficacy of 14 cloth masks, a surgical mask and an N95 found that a polyester/cotton blended mask and several cotton masks filtered out more than 80% of droplets, whereas knitted material and fleece filtered far less. There is also evidence that multi-layer cloth masks filter more efficiently than single-layer cloth masks.
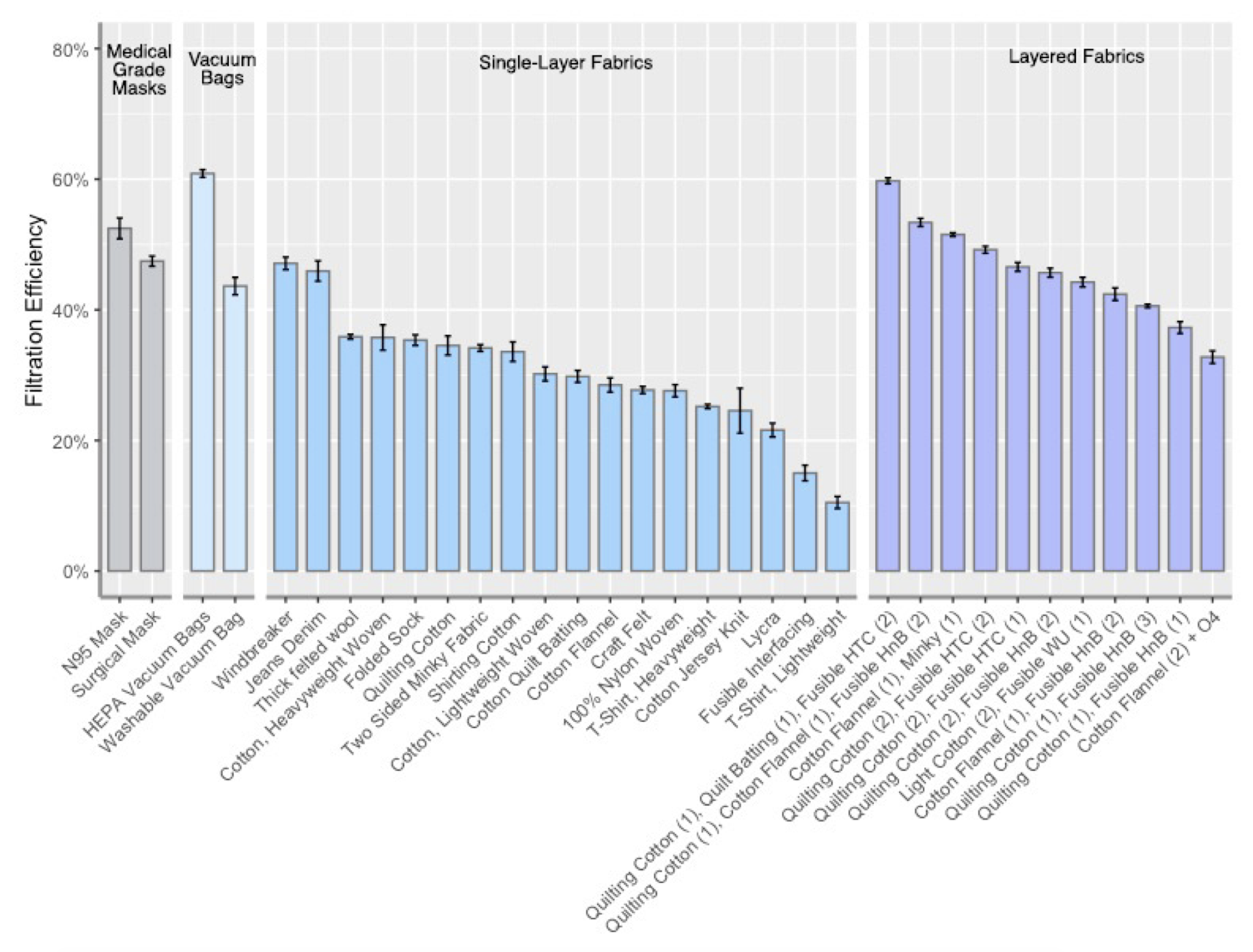
Source: BMJ Open
2) Evidence on the extent of asymptomatic spread and the importance of source control:
A mask can serve two functions: to prevent the spread of droplets from an infected person into the environment (“source control”) and to protect the wearer from exposure to droplets (personal protection). The fact that a significant proportion of SARS-CoV-2 infections are asymptomatic and viral loads are high during the presymptomatic phase of infection—before an infected person is aware they are ill—means that asymptomatic and presymptomatic people significantly contribute to transmission. In fact, models suggest that at least 50% of new SARS-CoV-2 infections may originate from exposure to individuals with infection but without symptoms. This provides a strong theoretical basis for widespread community mask use. Multiple studies have shown that some cloth masks, in particular those with several layers, efficiently block the release of droplets into the environment or limit their forward trajectory.
3) Evidence that masks other than respirators can efficiently protect the wearer:
Studies have shown that cloth masks can also protect the wearer from exposure to droplets. Some cloth masks have been shown to provide more droplet protection than surgical masks. For example, in a study that assessed the extent to which masks filtered particles that the wearer would otherwise have been exposed to, cloth masks displayed a range of filtration efficiencies (e.g., 79% for a 2-layer woven nylon mask; 50% for a multi-layered cotton bandana) but generally performed better than a surgical mask (39% filtration efficiency). This study also illustrated how much mask fit can affect mask performance. Surgical mask performance was improved with fit-enhancing modifications, listed here from highest to lowest filtration efficiency: adding a segment of nylon hosiery (80%); stretching rubber bands over the mask (78%); joining ear loops behind the head using a claw hair clip (65%); joining ear loops behind the head using an ear guard (62%); and tying ear loops and tucking in side pleats (60%).
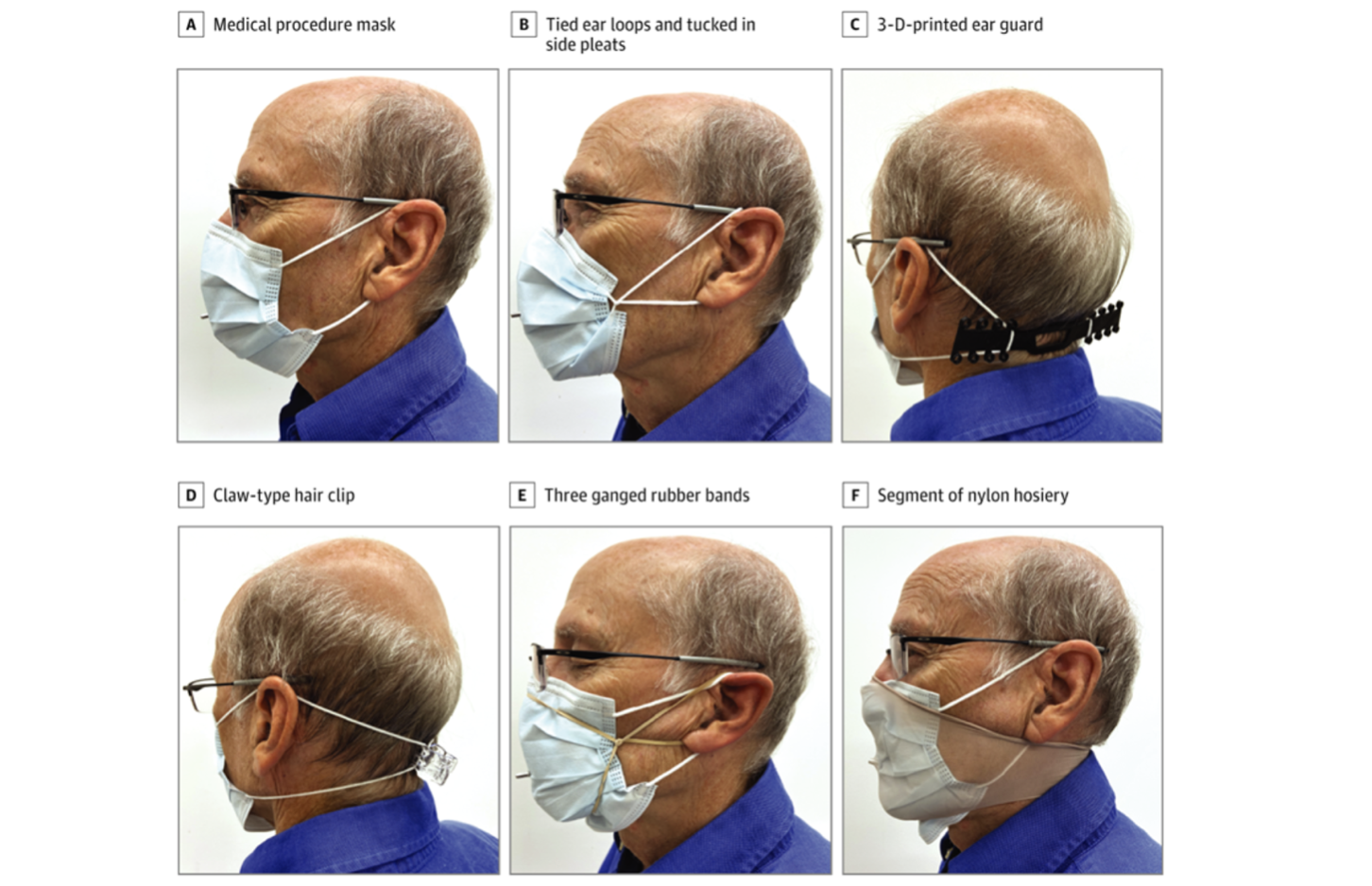
Source: JAMA Network
4) Evidence that when masks are worn in the community there is less transmission:
In order for a mask to reduce transmission as much as its filtration efficiency and ideal fit allows, it must also be worn correctly during all potential SARS-CoV-2 exposures. Thus, studies on the spread of COVID-19 in communities offer important insights on how the use of non-medical masks may decrease transmission. Much of the accumulated evidence that non-medical masks, or cloth masks, reduce the spread of COVID-19 in the community has been summarized in a recent CDC brief. Of particular note, a study conducted in Thailand after health authorities had recommended the use of cloth face masks in public showed that among over 1,000 people interviewed during contact tracing investigations, those who reported always wearing a mask during high-risk exposures had a 70% reduced risk of acquiring COVID-19 compared with those who did not report consistent mask use. On the USS Theodore Roosevelt, where an outbreak of COVID-19 infected over 1,000 people, self-reported use of face coverings was associated with a 70% reduced risk of disease. Analyses have shown that the implementation of mask mandates is associated with reduced spread of COVID-19 in multiple settings.
Respirators in the community: current recommendations and availability
There is renewed interest in whether filtering facepiece respirators (FFRs) such as N95 respirators should be used in the community. One driver is the emergence of new, more highly transmissible variants of SARS-CoV-2. In Brazil, South Africa and the United Kingdom, where these new variants likely emerged and now account for a significant proportion of cases, there are record numbers of cases, overwhelmed hospitals and increases in deaths despite attempts to control the spread of COVID-19. These three variants have now been detected in multiple other countries including the United States. It is clear that we must do more to prevent spread and there are questions about whether that includes more consistent wearing of masks by more people, the use of more effective masks in the community, or both. The new U.S. presidential administration has emphasized the importance of mask-wearing and issued executive orders mandating mask use in certain locations. Although FFRs have not been mandated, the use of N95s has been observed among staff in the White House. France has recommended the use of surgical masks in public while Germany and Austria have mandated the use of respirators in certain public places, citing new variants as a motivator.
Early in the pandemic there were reports of serious respirator shortages in U.S. health care settings. Various strategies to optimize supplies within health care settings were undertaken as the government partnered with respirator and mask manufacturers and increased the importation of N95s from other countries. Now, nearly a year into the pandemic, respirators for health care workers are still in short supply, with reports of limited access and the need to reuse single-use N95s. The extent to which non-N95 FFRs are being used in health care settings is unclear, but such FFRs are increasingly available for public purchase through multiple suppliers in the U.S. and there are examples of KN95 masks being given to the public for free. Outside the U.S., FFR supplies have been managed differently and demand is also different. In Germany, those over age 60 or with risk factors for severe COVID-19 are receiving vouchers for 15 FFRs each. In South Korea, FFRs were made available to citizens through government purchasing, distribution and rationing programs. The new U.S. presidential administration has directed agencies to address critical supply shortages, including mask shortages, using the Defense Production Act.
Given what we know and practical considerations, how should the public approach masking?
- When supplies are limited, the masks known to provide maximum protection to the wearer should preferentially be supplied to those at highest risk of acquiring COVID-19. The World Health Organization recommends that medical masks should be worn by health care workers or those caring for people with COVID-19, people with COVID-19 symptoms and people at high risk of severe COVID-19 when there is high community transmission and physical distancing cannot be maintained. In the U.S., the CDC continues to recommend against community use of medical masks because supplies should be conserved for health care workers. Ideally, those at highest risk of COVID-19 who most need the protection offered by respirators should undergo fit testing and use a respirator consistently during all potential exposures to SARS-CoV-2.
- Widespread community use of non-medical and surgical masks can reduce the spread of COVID-19 through both source control and protecting the wearer. However, not all masks are created equal. Data from studies on masks can be used to guide mask selection: masks should be made of non-woven material with a higher thread count and be composed of at least two layers of fabric. Some scientists and public health experts have recommended “double masking” to get the extra filtration offered by multiple layers. Masks with valves should not be used. When selecting a mask, fit is of utmost importance: the mask should completely cover the nose and mouth, tuck under the chin and fit snugly against the sides of the face to reduce air leakage.
- More concerted efforts to rigorously evaluate the real-world effectiveness of non-medical masks in the community are needed. It is possible that even without formal fit testing and with re-use, a filtering facepiece respirator (FFR) would protect the wearer more than even the most effective cloth mask, but it is also possible that a poorly fit N95 may perform worse than a well-fit, multi-layered cloth mask. The real-world difference in SARS-CoV-2 community transmission that FFRs would make, compared with high-quality cloth masks, is unknown. This is particularly true after accounting for factors that may influence mask efficacy (such as fit and reuse) and consistency of use (such as comfort, cost and availability). Fundamentally, the most important factor is whether a mask is worn; there is no evidence that transmission events have occurred because cloth masks were worn instead of FFRs.
- For masks to reduce transmission, they must be worn whenever there is potential for transmission of SARS-CoV-2. There has been appropriate emphasis on universal mask-wearing in public but it is also important to recognize the extent to which household transmission has contributed to the spread of COVID-19. Masks should also be worn in private indoor settings that involve people from more than one household. In addition, masks should be worn among household members if anyone has symptoms of COVID-19, has recently been in contact with someone with COVID-19 or has been diagnosed with COVID-19.
- No single intervention, including even most effective masks, can be relied on to eliminate transmission. A protective mask can reduce the likelihood of SARS-CoV-2 transmission but cannot eliminate risk. This is particularly true when a disease has more than one route of transmission. Any mask, no matter how efficient at filtration or how good the seal, does not obviate the importance of physical distancing, increased ventilation, hand hygiene and vaccination to prevent the spread of COVID-19.
FAQ: What is the CDC doing to track SARS-CoV-2 variants
All viruses mutate constantly as a result of “copying errors” that occur during the process of replication as a virus multiplies. Most mutations do not affect the virus’ core characteristics or how the virus behaves. Recently, several mutations have been identified in variants of SARS-CoV-2, the virus that causes COVID-19. These mutations have resulted in variants of the virus that may be more contagious, less likely to be covered by current COVID-19 vaccines and monoclonal antibody treatments, and possibly more deadly.
In order to monitor the emergence of new variants and identify how they may affect public health response, the U.S. Centers for Disease Control and Prevention (CDC) launched the SARS-CoV-2 Sequencing for Public Health Emergency Response, Epidemiology and Surveillance (SPHERES) consortium in May 2020. Through partnerships with state and local public health departments, research institutes, private laboratories and academic institutions, the CDC has been systematically collecting samples from across the country to evaluate with advanced molecular detection techniques. These techniques include mapping the entire genetic sequence of the virus in each sample and using bioinformatic analysis to identify changes in the virus. This information can then be used for epidemiologic analysis to determine if new variants are arising and if their behavior is different. If a new strain is identified, and the new strain is responsible for an increasing proportion of new infections over time, this may be a sign that the new strain has an evolutionary advantage over existing strains, such as increased infectiousness or ability to evade immune responses, which enables it to spread faster.
More recently, in response to reports of new variants, the CDC scaled its National SARS-CoV-2 Strain Surveillance program that originally started in November 2020 to process 750 samples a week from across the country. In addition, commercial labs in the U.S. are performing sequencing analysis of about 1,750 samples a week to help detect new variants. State public health labs, which have varying capacities to conduct whole genome sequencing, are also contributing to this process. As of early January, California’s state lab had sequenced almost 10,000 samples. In December 2020, the CDC released $15 million to state and local health departments to further support sequencing efforts. Experts are pushing for better strain surveillance and detection of variants in the U.S. to stay ahead of virus mutations that could affect disease spread and have major implications for vaccine manufacturers and vaccination programs.
Weekly Research Highlights
COVID-19 Cases and Transmission in 17 K–12 Schools—Wood County, Wisconsin, August 31–November 29, 2020
MMWR Early Release Jan. 29, 2021
- In Wood County (pop. 73,000), Wisconsin, 4,876 students and 654 staff members at 17 public and private schools contributed data to this 13-week study. Masking was required for all students and staff members at all schools, and the rate of reported student mask-wearing was >92%. Classroom cohorts consisted of 11-20 children. No systematic COVID-19 screening was conducted in the schools or the community.
- A total of 3,393 COVID-19 cases were reported in Wood County (cumulative incidence = 5,466 per 100,000 persons), including 191 cases within the participating schools (cumulative incidence = 3,454 per 100,000).
- Cases occurred in 133 students and 58 staff members. Among these 191 cases, seven (3.7%) were attributed to in-school SARS-CoV-2 transmission and all occurred among students. No in-school transmission between separate classroom cohorts was reported.
- Limitations included that asymptomatic transmission within schools could not be ruled out because surveillance testing was not conducted; the higher incidence of cases among staff than students may indicate that asymptomatic transmission from students to teachers occurred undetected. Mask use rates were self-reported; sources of infection were ascertained through contact tracing and not genomic sequencing; and results may not be generalizable to schools in other, non-rural settings.
New vaccine efficacy announcements
On Jan. 29, 2021, Novavax released interim efficacy results for its COVID-19 vaccine based on a phase 3 trial in the U.K. and a phase 2b trial in South Africa; both trials enrolled people 18-84 years old.
The 2-dose vaccine regimen, which is stable at refrigerator temperatures, showed nearly 90% efficacy in a 15,000 person trial in the United Kingdom. Half of the COVID-19 cases in the trial were caused by the B.1.1.7 variant. The efficacy dropped to 50% in a smaller trial in South Africa where almost all COVID-19 cases in the study were caused by the B.1.351 variant, suggesting that the vaccine provides lower protection against this variant. Vaccine efficacy was also lower overall among people with HIV. The manufacturer has begun clinical development of a booster or other vaccine to improve its efficacy for SARS-CoV-2 variants. Safety was comparable in the vaccine portion and placebo portion of the trials.
- In the U.K. trial, the vaccine demonstrated 89.3% efficacy (95% CI: 75.2 – 95.4). About 50% of cases in this trial were due to the B.1.1.7 variant, which was first identified in the U.K. and is now the predominant variant there. The other half of the COVID-19 events were due to non-variant strains of SARS-CoV-2. Additional analysis of these interim results will be forthcoming.
- Adverse events occurred at low levels and were balanced between vaccine and placebo groups.
- No severe cases of COVID-19 cases occurred in either trial among those who received the vaccine as a part of the study. In each location, one severe case happened among those who received the placebo.
- In the South Africa trial, the vaccine demonstrated an overall efficacy of 49.4% (95% CI: 6.1 – 72.8). Among the 94% of the study population that was HIV negative, the vaccine had an efficacy of 60% (95% CI: 19.9 – 80.1). Genomic sequencing was performed on SARS-CoV-2 isolated from 27 of 44 COVID-19 patents in the trial, and 25 of these 27 (92.6%) cases were caused by the B.1.351 variant, first identified in South Africa. Despite some evidence of protection against this variant, Novavax began planning for new variants in January, and will start clinical development of a booster of bivalent vaccine, or vaccine that stimulates the immune system against two different variants, during the second quarter of 2021.
- One in three patients enrolled in the South Africa trial had antibodies against SARS-CoV-2 upon enrollment (not included in above analysis). Novavax asserts that its vaccine-induced immunity may offer better protection against the B.1.351 variant than natural immunity after non-variant SARS-CoV-2 infection.
- Novavax continues to recruit for its Phase 3 trial in the U.S. and Mexico.
- NVX-CoV2373, Novavax’s vaccine, is a 2-dose recombinant SARS-CoV-2 vaccine with a proprietary adjuvant (Matrix-M) to boost the immune response. The vaccine can be stored and transported at refrigeration temperatures (2-8 degrees Celsius, 36–46 degrees Fahrenheit) and does not require reconstitution at the point of administration.
- Novavax hopes to produce two billion doses of vaccine this year, with a large portion of this supply earmarked for low- and middle-income countries.
On Jan. 29 2021, Johnson & Johnson (J&J) released interim efficacy results for its single-dose adenovector COVID-19 vaccine based on data from a phase 3 trial that enrolled adults 18 years and older.
The study, which included sites in the U.S., South Africa and Latin America, demonstrated an overall vaccine efficacy of 66% against moderate to severe COVID-19. Unlike J&J, other manufacturers (Pfizer/BioNTech, Moderna, Novavax) have been collecting and reporting efficacy data against all symptomatic COVID-19 (mild, moderate and severe). Since COVID-19 vaccines have been shown to be more effective at preventing more severe cases of disease, J&J’s vaccine likely may have had less than 66% efficacy if the efficacy against COVID-19 of any severity had been assessed. This should be taken into account when conducting head-to-head comparisons of J&J’s vaccine efficacy data against data on other vaccines. It should also be considered that a single dose of the J&J vaccine has a similar efficacy to reported efficacy after a single dose of two-dose mRNA vaccines currently authorized for use. The company also reported that efficacy varied by geographic location, suggesting that efficacy may be reduced in locations with some newly identified variants of SARS-CoV-2. Efficacy was higher in the U.S. (72%) and lower in South Africa (57%), where almost all of the COVID-19 events were caused by the B.1.351 variant. The vaccine was well-tolerated and serious adverse events were reported more frequently in participants who received placebo than in participants who received the vaccine. The manufacturer continues to investigate a 2-dose regimen of its vaccine in a separate study and plans to apply for emergency use authorization of its single-dose regimen in the U.S.
- More than 43,000 people at multiple sites are enrolled in J&J’s phase 2 ENSEMBLE study. Results were released after reaching primary endpoints to evaluate efficacy.
- Vaccine efficacy was first evaluated at 14 days, the time point at which evidence of antibody protection was seen. Efficacy data are based on events up to 28 days post-vaccination. In a previous publication, antibodies had continued to build over time and reached their highest level at 57 days after vaccination.
- Overall efficacy was 66% for protecting against moderate to severe disease and there was regional variation: efficacy was 72% in the U.S., 66% in Latin America, and 57% in South Africa. These data raise concern about vaccine efficacy against variants. Study sites included Brazil, where the P.1 variant was first reported, and South Africa, where the B.1.351 variant was first reported.
- Unlike other manufacturers, J&J is focusing on efficacy to protect against moderate and severe disease. Other manufacturers have reported efficacy against all COVID-19 severities (mild, moderate and severe disease). The company reported 85% efficacy in protecting against severe COVID-19.
- A significant proportion of study participants reported at least one comorbidity (41%), including obesity (28.5%), type 2 diabetes (7.3%), hypertension (10.3%) and HIV (2.8%).
- No significant differences were seen in protection among different racial and age groups. More than 13,000 enrollees were over age 60.
- The vaccine, which uses the company’s proprietary AdVac technology (also used in J&J’s Ebola virus vaccine), can remain stable at freezer temperatures (-4C or -20F) for two years and at refrigerator temperatures for three months.
- Last November, J&J started its ENSEMBLE 2 study, in which it is evaluating a 2-dose regimen of its vaccine. There have not been official comments regarding boosters or a multivalent vaccine to address emerging variant
Suggested citation: Cash-Goldwasser S, Kardooni S, Cobb L, Bochner A, Bradford E and Frieden TR. Weekly COVID-19 Science Review January 16-29, 2021. Resolve to Save Lives. 2021 February 2. Available from https://preventepidemics.org/coronavirus/weekly-science-review/. In-Depth COVID-19 Science Review January 16 – 29, 2021. Resolve to Save Lives. 2021 February 2. Available from https://preventepidemics.org/covid19/science/review/





