Download All Country Data
Even under optimal circumstances, it is challenging for health care workers (HCW) to stay up to date on the latest public health guidelines and best clinical practices. The COVID-19 pandemic brought about a flood of new guidance along with restrictions on travel and gathering. Organizations worldwide had to adapt to a new normal that exacerbated the difficulties of delivering effective and engaging HCW training — right when such guidance was needed most.
At the start of the pandemic, the Prevent Epidemics team at Resolve to Save Lives (RTSL) launched a new program to support partner organizations in Africa with HCW training and mentorship in primary health care facilities. The program focused on making health facilities safer and limiting the spread of COVID-19 in health care settings. The training component of the program focused on infection prevention and control (IPC) – the evidence-based practices used to protect HCW and their patients to prevent the spread of avoidable infections.
RTSL searched for online courses to supplement the HCW program’s in-person training activities but found that many existing courses were not optimized for use by HCW. Some of the courses covered content that wasn’t relevant, or were offered on platforms that were difficult to use on a smartphone — the primary means of accessing the internet for many HCW in Africa. Finally, many of the courses asked students to learn by watching video lectures, a passive process that doesn’t foster as much learning as interactive approaches that involve answering questions and solving problems.
Self-paced infection prevention and control training
To provide its partners with an additional training tool, RTSL developed an online IPC course for HCW working in primary health facilities. The course consists of realistic case scenarios delivered in short modules. Learners are asked questions about how health facility staff should respond in each case and receive immediate feedback as they progress. This approach continuously engages users in the learning process — and is more effective than simply offering text to read or videos to watch. Although the course focuses on basic IPC knowledge, clinical cases anchor the learning to health care workers’ day-to-day activities.

An illustration used in the course
The IPC course was created in close collaboration with colleagues at the African Field Epidemiology Network (AFENET) and the Nigeria Primary Health Care Development Agency (NPHCDA). All course content was based on World Health Organization (WHO) guidance and closely aligned with national guidelines in Nigeria. The characters in the cases are nurses, doctors and other staff working in primary health care facilities, all with names that are common in Nigeria.
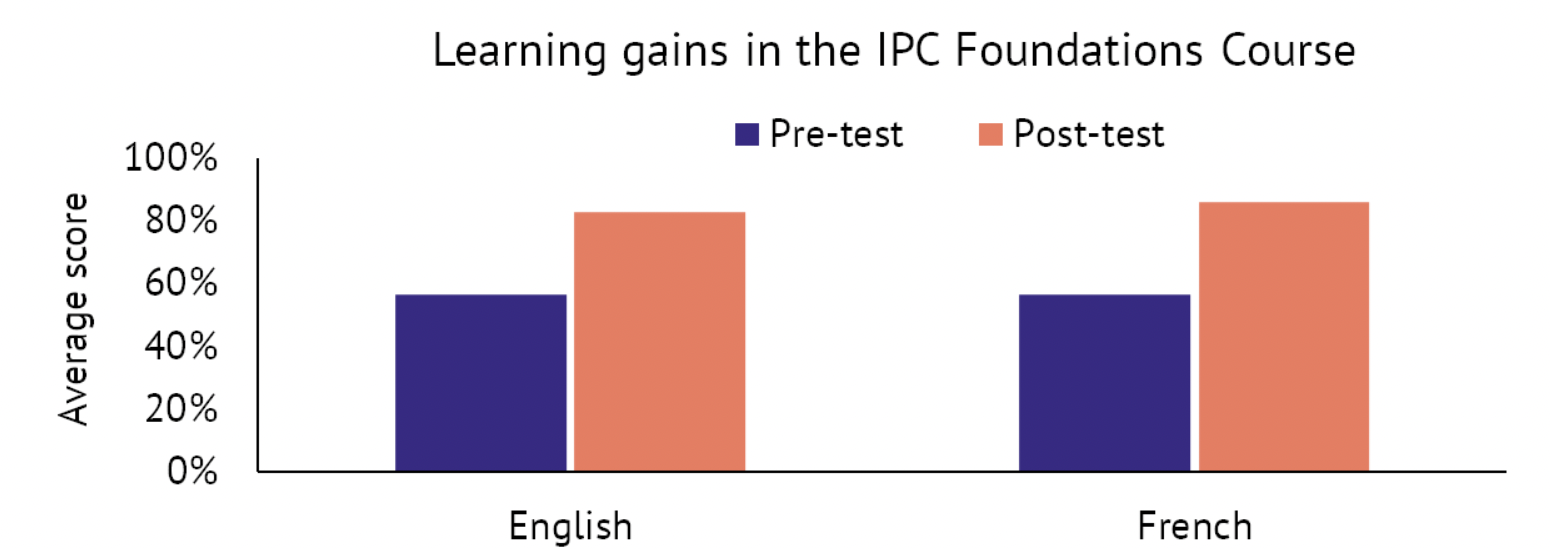
Partnering with AFENET, RTSL piloted an English version of the course in Nigeria. At the end of the pilot, 372 health workers had enrolled in the course. The overall results were quite positive: 59% of enrollees completed the course, those who completed the course improved their knowledge of IPC as measured by a pre-test with a matched post-test, and learners provided very positive feedback on the course. An evaluation of this first pilot of the course was recently published in BMC Public Health.
First steps to scale
To build off this early success, RTSL set the more ambitious goal of offering the IPC course in multiple countries and in two languages (English and French). Using data from the first course run, the team identified areas where the course could be improved and made updates. This new version of the course was offered across Africa in late 2021.
With these promising early results in hand, RTSL is offering the IPC course again, along with a new course that helps HCW build the skills they need to advocate for safe workplaces. The new course builds on short and engaging animated videos created by the Digital Medic initiative at the Stanford Center for Health Education and the Community Health Impact Coalition.
Lessons learned
RTSL attributes its initial success with the IPC course to focusing on the unique learning needs of HCW and making continuous improvements based on pilot results and learner feedback. The Prevent Epidemics team identified key features of effective HCW training that they applied in the design of the modules. The resulting training is:
- Focused and relevant: learning is driven by examples that are set in health care facilities and directly applicable to learners’ day-to-day work.
- Engaging: learning begins as quickly as possible, with HCW engaging in critical evaluation of clinical situations and receiving immediate feedback via brief explanations embedded in assessment questions.
- Mobile-optimized and low bandwidth: designed for mobile devices and for use over 3G connections.
- Widely accessible: does not require downloading new software, has a straightforward registration process and is offered free of charge.
- User-friendly and simple: has intuitive navigation with minimal menus and does not require any orientation for learners to get started.
- Self-paced and brief: broken into short modules that can be completed at the learner’s discretion.
“We wanted to create a better alternative – courses that would be engaging yet effective for learning,” says Jobin Abraham, Director of Learning and Capacity Development at Prevent Epidemics. “Health care workers face a variety of different barriers to learning online, and we aimed to address as many of those challenges as possible.”
Just as importantly, the team collaborated closely with partners to ensure that the solution filled a real gap and reached the target audience.
“This project has given us proof of concept that these case-based online courses can be effective for training health workers,” says Christopher Lee, Director of Global Epidemic Preparedness and Response at Prevent Epidemics. “The next step is to scale this up, and partnership is the pathway to scale. We see this as a promising tool for governments and NGOs to roll out new guidance and keep their health workforces up to date.”
For more information, read “Development of a simple and effective online training for health workers: results from a pilot in Nigeria,” published in BMC Public Health.

An illustration used in the course






