Download All Country Data
When Ghana recorded its first two COVID-19 cases in March 2020, the government took swift and decisive action to stop the spread. These efforts, which included lockdowns restricting social gathering and movement, as well as the closure of schools, workplaces and places of worship, came at the price of disrupting daily life on a grand scale.
The pandemic has hit health care workers particularly hard. One analysis estimates that at least 17,000 health care workers worldwide had died from COVID-19 as of March 5, 2021. Protecting them requires a range of interventions, including investing in training, tools and resources for a safer workforce and full implementation of infection prevention and control (IPC) and water, sanitation and hygiene (WASH) standards. Keeping health care workers safe is fundamental to a successful response effort; health care workers provide life-saving care to both patients suffering from COVID-19 and those that need to access other essential health services such as routine check-ups, medication refills, antenatal care and delivery.
In Ghana, as in much of the rest of the world, health care workers faced significant barriers to implementing new COVID-19 protocols. Analysis found that 77 percent of health facilities in Ghana lacked proper face masks, while half lacked surgical gloves. At certain facilities, health care workers provided care without adequate personal protective equipment (PPE) or adequate knowledge of IPC standards, resulting in COVID-19 transmission. At Sefwi-Wiawso Hospital in Ghana’s Western North Region, for example, multiple patients and health care workers tested positive for COVID-19.
Training health care workers on the frontlines of a pandemic
There was a clear need to provide training for health care workers on how to deliver services during COVID-19. Between September and December 2020, Jhpiego, a global health nonprofit affiliated with Johns Hopkins University and based in the United States, worked with the Ghana Health Service (GHS) to conduct a series of virtual trainings to develop the capacities of frontline health care workers to sustain essential services during the pandemic.
At the trainings, health care workers learned proper IPC protocols for COVID-19, including how to identify people with potential COVID-19 symptoms, how to develop a standard operating procedure for screening and triaging patients and how to administer COVID-19 testing. The trainings reached 944 primary and secondary health care workers across 186 health facilities in six regions: Greater Accra, Ashanti, Ahafo, Bono East, Western and Western North.

Samuel Adusei (left), IPC lead at Sefwi-Wiawso Hospital, demonstrates how to take PPE on and off a nurse.
The trainings were held via Zoom and shared via the GHS eLearning platform, which provides virtual trainings for all health workers in Ghana. Resolve to Save Lives (Resolve), an initiative of Vital Strategies, contributed modems, data and technical expertise to help facilitate the trainings; the United States Agency for International Development (USAID) funded the project in the Western Region. In January 2021, when the trainings were complete, Resolve distributed PPE including gowns, gloves, masks and hand sanitizer to the 186 facilities. These supplies helped protect health care workers and patients alike by contributing to their safety in the maintenance of non-COVID-related essential services such as routine check-ups and antenatal care.
Applying lessons learned
Across the 186 health facilities, there were noticeable improvements from the training’s start to its end. The percentage of facilities that had socially distanced triage and screening areas increased from 53 percent to 75 percent. At the outset of the training, 42 percent of the facilities had adequate quantities of surgical masks; by the end, this number had jumped to 88 percent.
Facilities also implemented specific best practices from the trainings. At Sefwi-Wiawso Hospital and at Princess Marie Louise Children’s Hospital in Accra, for example, several Veronica Buckets, which are portable hand-washing stations that use running water, are now available for incoming patients to wash their hands without risk of contamination. At each entrance, a nurse is stationed close to a designated triage area to engage incoming patients with routine questions and check their temperature to assess possible COVID-19 symptoms. Each hospital also organized refresher trainings on water, sanitation and hygiene (WASH), social distancing and PPE usage.
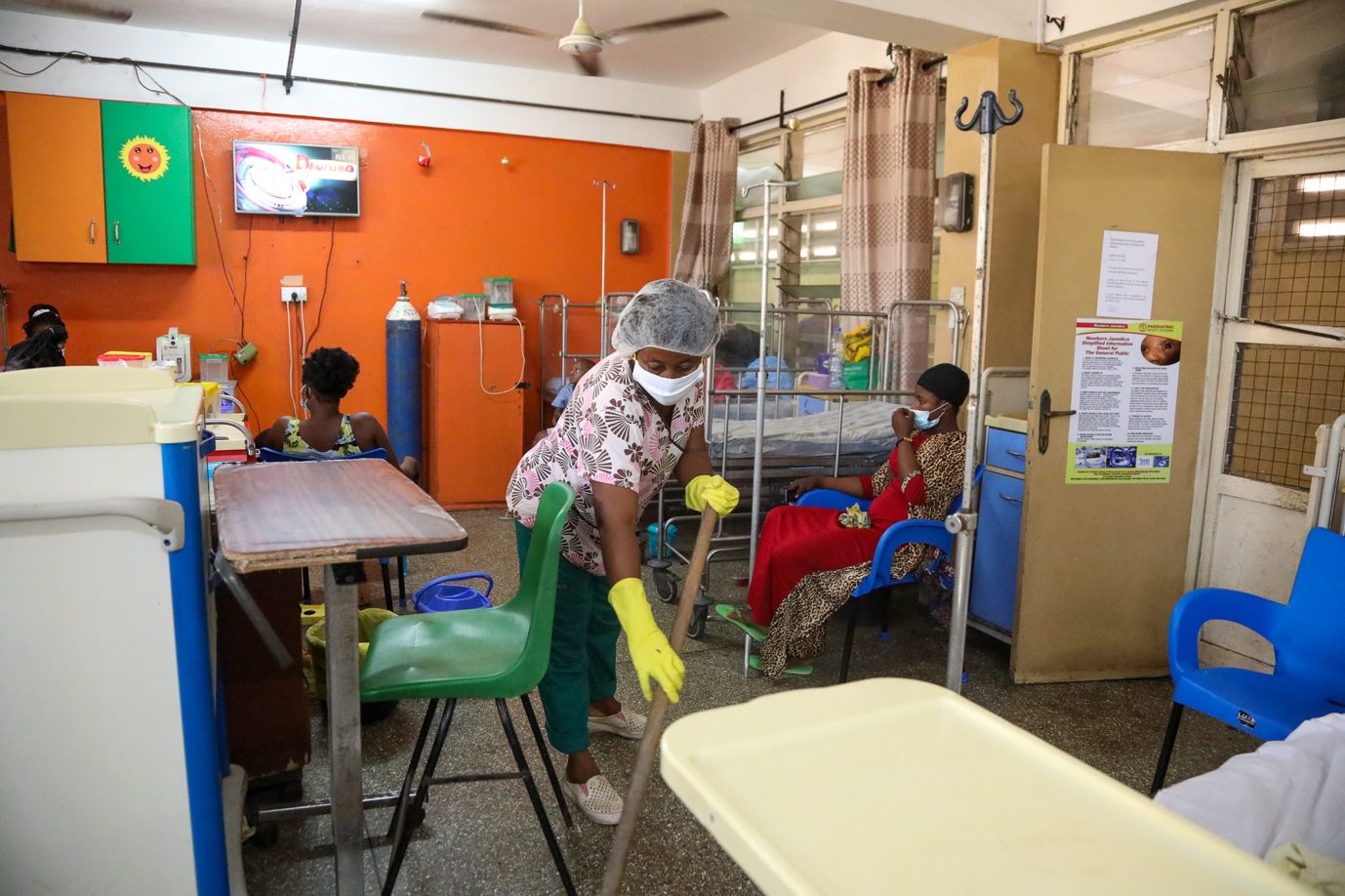
An orderly trained in proper IPC protocols cleans wards with a chlorine solution at Princess Marie Louise Children’s Hospital.
“We now have IPC focal persons for every department, ward and unit that we trained to train their colleagues on the job and encourage adherence to IPC standards, as well as ensure regular supply of PPE from the store,” said Samuel Adusei, a mental health nurse at Sefwi-Wiawso Hospital.
As a result of the trainings, certain hospitals also reevaluated how they offer care to special needs patients during the pandemic. To limit potential exposure, the staff at Princess Marie Louise Children’s Hospital now recommends patients in child welfare and sickle cell clinics, for example, visit once every two months instead of monthly. The hospital has scheduled voice calls to regularly check on such patients and arrange visits when necessary.
The trainings also touched on the importance of maintaining one’s physical, emotional and mental health. The everyday stress of being a health care worker is immense and is only exacerbated by a pandemic; one review of the psychological impact of epidemics found that many health care workers exhibit symptoms in keeping with post-traumatic stress disorder (PTSD).
“To be able to care for our client, we must first take care of ourselves,” said Samuel Nkrumah, a nursing officer and the IPC lead at Princess Marie Louise Children’s Hospital.
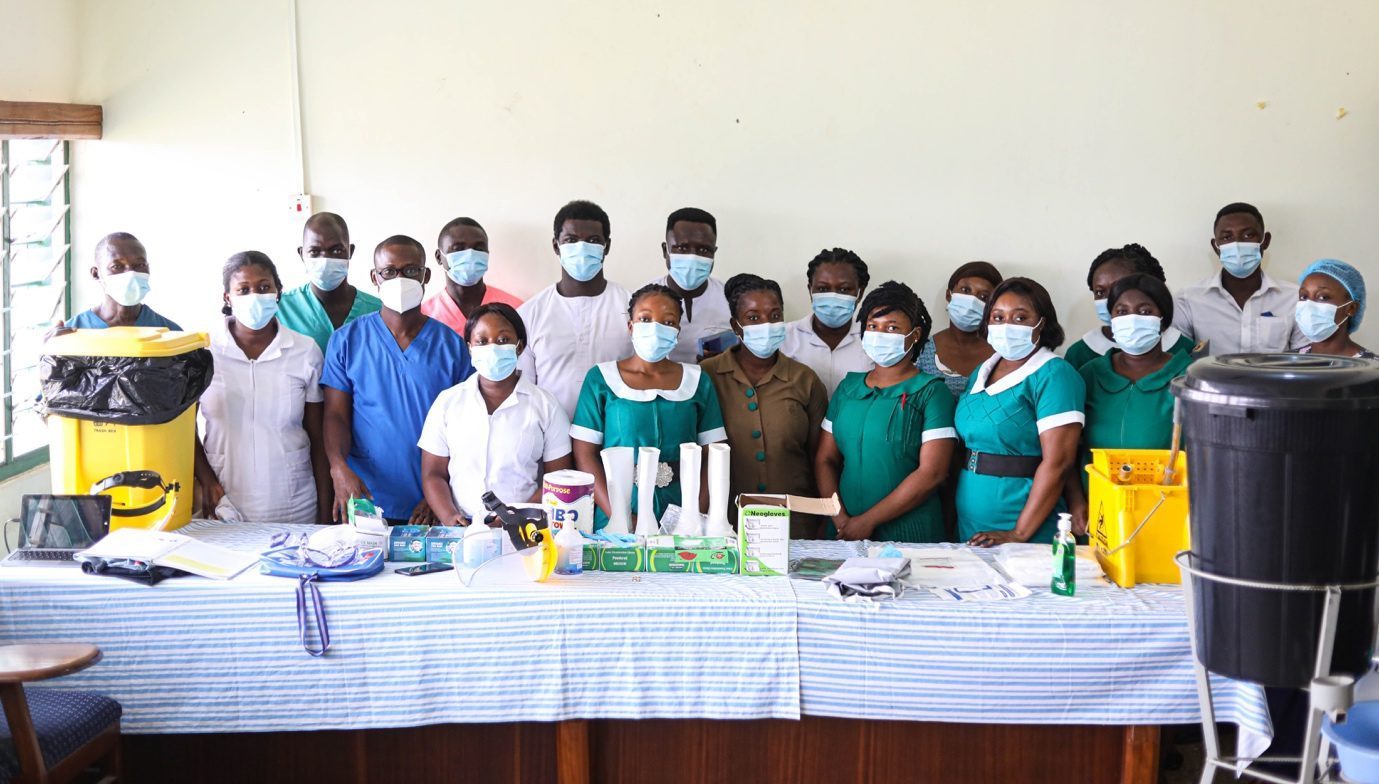
IPC leads from Sefwi-Wiawso Hospital






