A national COVID-19 alert level framework
Alert-level systems should form a core component of effective COVID-19 preparedness and response. We propose that the United States introduce a national framework for a COVID-19 alert-level system that can be adapted and implemented locally. An alert-level system can inform communities about the local risk of COVID-19 and empower them to stay safe. If designed effectively and linked to guidance on public health and social measures appropriate for different disease transmission levels, an alert-level system can prevent a scenario where the burden of COVID-19 is so high that the most disruptive mitigation measures become necessary to relieve an overloaded health care system. An alert-level system should be built on a solid base of scientific evidence that can be applied nationally. However, alert-level systems must be implemented locally, taking into account the local economic, political and social context. When implemented effectively, an alert-level system can reduce COVID-19 transmission and save lives.
See our proposal for a national COVID-19 alert level framework here.
Restaurant dining and COVID-19
The data indicating that indoor dining is a higher-risk activity has amassed from a variety of sources. At the foundation, there are principles of disease transmission—of which our understanding has greatly evolved over time—that provide the basis for plausibility as to why restaurants may be risky environments. Next, there are observational studies from contact tracing programs that examine the various types of exposures reported by cases. Indoor dining often stands out in these types of reports as a common exposure among those who have become infected. Then, there are case-control studies, in which exposures are evaluated more systematically to hone in on a common source of infection or behavior that may be affecting those who become sick. Finally, there are epidemiologic models that look at the impact of restaurant openings and closures and extrapolate from mobility data and traffic to restaurants, estimating how levels of infection may change depending on the number of people visiting restaurants.
Brief review of principles of disease transmission and limiting spread
SARS-CoV-2 is a virus that primarily spreads from person to person through respiratory particles. This can happen through close contact at shorter distances (generally up to six feet) as a result of larger particles (often called droplets) that carry the virus being expelled by one person and inhaled by another. Transmission can also occur as a result of smaller particles that can travel longer distances (produced during activities such as singing, speaking loudly or exercising) that may linger in the air longer due to poor ventilation (referred to as airborne transmission). As with other respiratory viruses, it is also possible that a person may come into contact with the virus either through direct contact with an infectious person (e.g., shaking hands) or by touching something contaminated with the virus (e.g., high-touch surface such as a door handle) and then touching their mouth, nose or eyes. Over time, it has become evident that surfaces likely play a lesser role in the transmission of SARS-CoV-2. However, it is important to reduce this lesser risk by avoiding sharing items and following enhanced cleaning procedures, particularly for commonly-touched surfaces such as door handles and elevator buttons.
The principles of preventing disease spread, referred to as the 3 W’s, address the aforementioned modes of transmission: wearing a mask is designed to both limit exposing others to expelled or exhaled virus from an infected person and limit the amount of virus an uninfected person may inhale; watching distance is designed to decrease the risk of being exposed to a respiratory particle that may be carrying the virus and minimize close contact with others, and washing hands is designed to prevent spread of virus through contact with common surfaces and shared items.
Risky COVID-19 behaviors are inherent to restaurant dining
With these principles in mind and thinking about an indoor dining experience, it can quickly become clear how the environment is one that has heightened risk factors for COVID-19 transmission, while simultaneously limiting the ways that people can protect themselves and others to reduce spread. Studies have found that outside of the household setting, which has the highest risk of secondary infection (covered here in a previous weekly science review), social settings such as restaurants pose the highest risk for disease transmission due in part to the increased number of close contacts. In restaurants, people cannot always maintain a safe distance from others while being served and interacting with waitstaff. They cannot always avoid passing by other tables of unmasked diners speaking loudly to overcome the ambient background noise—a behavior that may lead to increased airborne transmission. People cannot wear masks consistently while eating. They also cannot always limit sharing or touching common items such as bottles of water, plates of food, tables and chairs, all of which have been handled or touched by another person outside the dining party without an opportunity for cleaning or hand hygiene in between. The increase in risk from these behaviors is amplified further in indoor environments with decreased ventilation, a setting known to be higher risk at baseline for COVID-19 transmission. This is reflected in the most up-to-date guidance from the U.S. Centers for Disease Control and Prevention (CDC), which lists indoor dining with reduced-capacity seating and at-capacity seating as higher and highest risk respectively for patrons of restaurants and bars. Although the focus of much of the research about restaurants is on patrons, the increased risk to staff and food-service workers should not be overlooked.
Linking restaurant dining to increased disease incidence
In one study, researchers used a sophisticated model informed by mobility data; visits to points of interest such as restaurants, places of worship or grocery stores; census block data and observed new infections over time. They then analyzed these data in several ways to assign risk for infection based on the type of point of interest. In their analysis, after sectors began reopening following the initial wave of stay-at-home orders, visits to full-service restaurants where indoor dining was allowed was by far the riskiest type of venue to visit. In the Chicago area alone, the researchers estimated that after reopening restaurants for full service, there were almost 600,000 additional infections by the end of May linked to people visiting and patronising these establishments. Based on mobility data, they were able to predict that restaurants were of higher risk at least in part due to full-service restaurants having higher numbers of visits which each lasted a substantial amount of time, increasing chances for exposure and disease transmission.
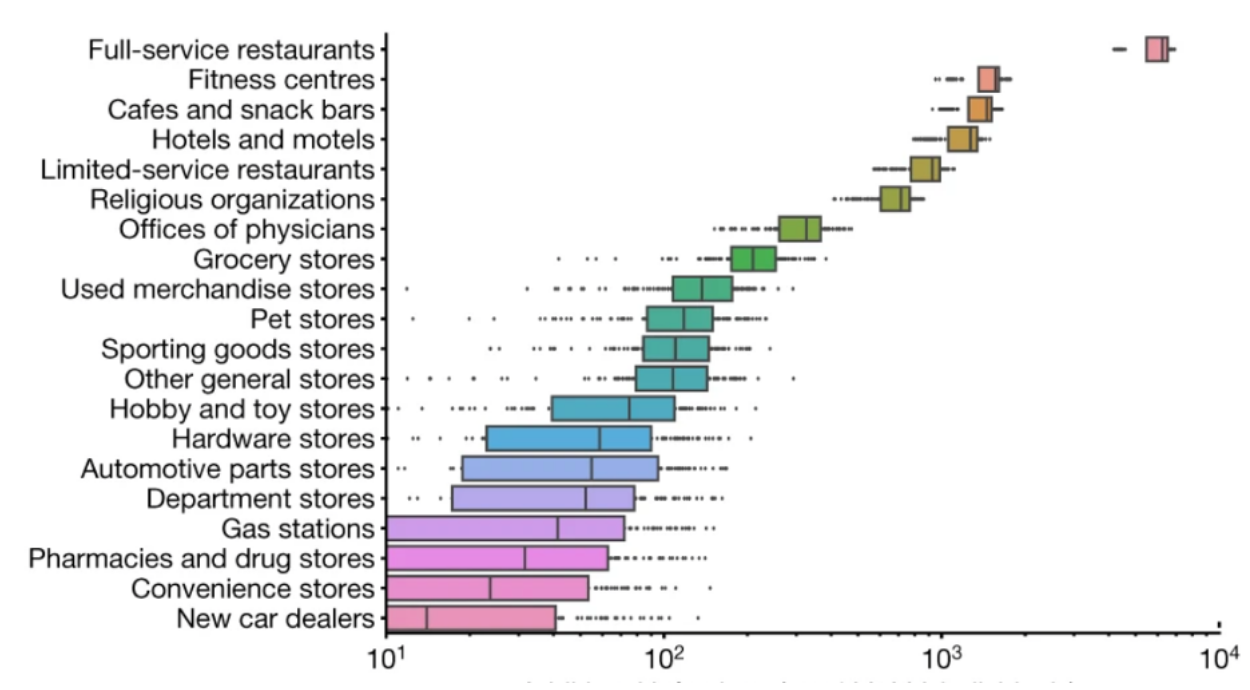
Source: Chang et al. Nature
In addition to individual reports with direct evidence of infection transmission occurring in restaurants, such as the report of the first cluster of cases of COVID-19 in Indonesia being linked back to a restaurant, there has also been other epidemiologic reporting on this topic. In September, a Weekly Morbidity and Mortality Report from the CDC found that among a group of cases who tested positive for COVID-19 and controls, the cases were twice as likely to have visited a restaurant for on-site dining in the two weeks prior to testing positive. In August, the New York Times reported on analysis of state data that linked 12% of COVID-19 cases in Maryland and 9% in Colorado to restaurants. In another report from Los Angeles, though the data used for analysis was not provided, the health commissioner reported that in October, almost one-sixth of all cases being diagnosed in the area were linked to a “dining experience.” Other reports of outbreaks linked to restaurants are numerous with examples from across the country. The directionality of disease spread—whether it is spreading primarily from staff to patrons, among patrons and staff, or all of the above—is more difficult to determine. Other matters that can make tracing the source of infection more difficult in restaurants and other indoor spaces are directionality of air flow, as was discussed in a recent study from Korea. In this study, directed air flow from an infected person resulted in transmission of disease after just 5 minutes of exposure at a distance greater than six feet. Indoor air current resulting in transmission at a restaurant has been implicated before in a restaurant in China.
Reducing capacity and mitigating risks of restaurant dining
The Infectious Disease Society of America rates indoor dining at a restaurant as “high risk,” outdoor dining at a restaurant as “medium risk,” and getting takeout from a restaurant as “low risk.” There are some steps that establishments can take to reduce the risks of indoor dining. These include distancing tables at least six feet from one another, replacing high-touch items such as menus with virtual versions and improving indoor ventilation through enhanced HVAC settings and air filtration when possible. Reducing ambient noise volume (to reduce the volume of speech) and encouraging diners to use masks when not eating can also help. The exact amount that each of these steps may help reduce transmission of COVID-19 has yet to be quantified. What has been studied more are the benefits of reducing capacity and using reservations to keep the overall number of visitors as high as possible while reducing the number of diners in the establishment at any given time. The modeling study cited earlier found that by reducing capacity to 20%, a significant proportion of infections could be prevented, while minimizing economic disruption and avoiding completely closing a sector that has already been hard-hit by the pandemic, especially smaller and locally owned establishments.
With disease transmission at the levels that the U.S. is currently experiencing, another wave of restaurant closures has already started in major metropolitan areas. Now almost a full year after the first case of COVID-19 was formally identified in Wuhan, China, the pandemic is causing its most severe impacts in some parts of the world and much of the U.S. Although no single industry is responsible for the magnitude of the pandemic in the U.S., on-site dining at restaurants, especially indoors, continues to be a common higher-risk activity that makes a large contribution to overall disease transmission and should be limited and avoided until community transmission is more under control. Individuals and communities can all do their part to reduce overall disease transmission and keep economies as open as possible by continually supporting restaurants and food outlets through takeout and delivery service when dining in is not safe enough. For further information on how restaurants and other sectors can incorporate capacity limits and other ways to reduce disease spread at different levels of disease activity, see our proposal for a national alert-level system.
What is the Ellume COVID-19 Home Test, a new fully-at-home COVID-19 test?
On Dec. 15, 2020, the U.S. Food and Drug Administration (FDA) issued an emergency use authorization for the first COVID-19 test that can be purchased over the counter and completed at home. The Ellume COVID-19 Home Test, an antigen test that can diagnose COVID-19 by detecting proteins expressed by the virus, works using technology that is similar to other rapid tests that can be done in provider offices (rapid-flu and rapid-COVID tests) and at home (pregnancy tests). It is the first COVID-19 test that can be run and resulted by consumers fully at home without needing a prescription or sending a sample to a laboratory for processing.
The test is expected to arrive at U.S. pharmacies in January 2021, and to cost $30 or less. The Ellume COVID-19 Home Test can provide test results in 15 minutes, and is authorized for use in people with and without symptoms. It can be used in people as young as 2 years old. It comes in a kit that includes a sterile nasal swab to collect a sample for testing, a dropper and processing fluid to prepare the sample, and a Bluetooth enabled analyzer that connects the test kit to the user’s smartphone through a dedicated app, which also provides step-by-step instructions and displays the test result. The test kit is set up to share test results in a HIPAA compliant manner with a user’s medical provider or relevant public health authorities through its app, where applicable.
In a clinical study of 200 people to see how accurately the test showed positive and negative results compared to a lab-based PCR test, the Ellume test was accurate 95% of the time for positive tests and 97% of the time for negative tests. The test performs better in people with symptoms compared to those without symptoms: for people with symptoms, the test kit correctly identified 96% of positive samples and 100% of negative samples whereas for people without symptoms, it correctly identified 91% of positive results and 96% of negative results. This reported performance is better than many other antigen tests currently in use at provider offices. Although its supply is expected to be somewhat limited, adding some 20 million tests to the market in the first half of 2021, it is the first example of a test that can be handled completely by the user and expands access to testing.
Weekly Research Highlights
Household Transmission of SARS-CoV-2: A Systematic Review and Meta-analysis
(JAMA, Dec. 14, 2020)
- Household attack rates ranged from 45% in a study in Italy to 0% in a study in South Korea. Attack rates did not differ significantly between studies conducted in China when compared to other countries, studies conducted in January and February compared to March through July, or between higher and lower quality studies.
- In the seven studies that examined the type of household contact, spouses were significantly more likely to test positive (37.8%; 95% CI: 25.8 – 50.5%) compared to other household or family contacts (17.8%; 95% CI: 11.7 – 24.8%).
- Asymptomatic or presymptomatic index cases were examined in only four studies; however, the attack rate from these studies was 0.7% (95%CI: 0 – 4.9%) compared to 18% (95% CI: 14.2 – 22.1%) among symptomatic index cases.
- From the seven studies that reported relevant information, the authors found that COVID-19 infections were not evenly spread across households but showed a tendency to cluster (e.g., some households reported everyone tested positive for COVID-19 while others had no one test positive).
- Critical illness in the index patient may also be associated with increased infectiousness; this association was statistically significant in six of the nine studies examined.
- Limitations included the fact that 18 of the included studies only tested symptomatic contacts for COVID-19 and many studies could not distinguish between secondary transmission in the household and community transmission. Further, while the meta-analysis included 54 studies, only a limited number looked at key questions such as infectiousness of children compared to adults.
Vaccines That Prevent SARS-CoV-2 Transmission May Prevent or Dampen a Spring Wave of COVID-19 Cases and Deaths in 2021
(MedRxiv preprint, Dec. 14, 2020)
- The authors used a mathematical model developed with data from King County, Washington that projects the trajectory of the pandemic through the end of 2021. Without a vaccine, this model predicts a large fourth wave of infections between April and October 2021. Using this model, the authors estimated how several different vaccine profiles would impact the projected number of COVID-19 cases, hospitalizations and deaths through the end of 2021.
- The authors found that a vaccine with only 10% efficacy at preventing infection, but with a 90% efficacy at preventing symptoms, would avert a large fourth wave of COVID-19 cases if the vaccine leads to a 50% or greater reduction in infectiousness. Only a 10% or greater reduction in infectiousness would be needed to prevent most deaths during this fourth wave assuming that the vaccine is prioritized for the elderly population.
- Were vaccine rollout slower than anticipated, the mechanism through which the vaccine prevents symptomatic infections would have a larger impact on the ability of the vaccine to prevent the fourth wave of the epidemic. The model also shows the vaccine having a limited impact on the ongoing third wave of COVID-19, and that the size of this current wave will depend on human behavior.
- These results rely on several assumptions, including the speed of vaccine rollout, the long-term efficacy of the vaccine and uncertainty around human behavior that will affect the trajectory of the COVID-19 epidemic
Evaluation of Cloth Masks and Modified Procedure Masks as Personal Protective Equipment for the Public During the COVID-19 Pandemic
(JAMA Internal Medicine, Dec. 10, 2020)
- Investigators measured the fitted filtration efficiency (FFE) of five medical and seven non-medical masks. An adult male volunteer with no beard wore the masks while performing movements of the torso, head, and facial muscles stipulated in national mask assessment guidelines. Popular mask modifications, including enhancements with rubber bands and nylon hosiery, were also tested on the medical masks. The FFE was tested by generating aerosolized particles of sodium chloride around the participant’s head and comparing the sodium chloride concentrations in air samples collected inside and outside each mask.

- Non-medical masks had a wide range of mean FFEs, listed from highest to lowest: (1) 2-layer woven nylon mask with a nose bridge (79%); (2) cotton bandana folded into a multilayer rectangle per a public health message from the U.S. Surgeon General (50%) or (3) folded diagonally (49%); (4) single-layer woven polyester/nylon mask (38%); (5) single-layer woven polyester gaiter (38%); (6) nonwoven polypropylene mask (28%); and (7) 3-layer woven cotton mask (27%).
- Medical procedure masks had a mean FFE of 39%, lower than most of the non-medical masks. Modifications increased medical mask FFEs as follows, listed from highest to lowest: (1) segment of nylon hosiery (80%); (2) three ganged rubber bands (78%); (3) ear loops joined behind the head using a claw-type hair clip (65%); (4) ear loops joined behind the head using an ear guard (62%); and (5) tied ear loops and side pleats tucked in (60%).
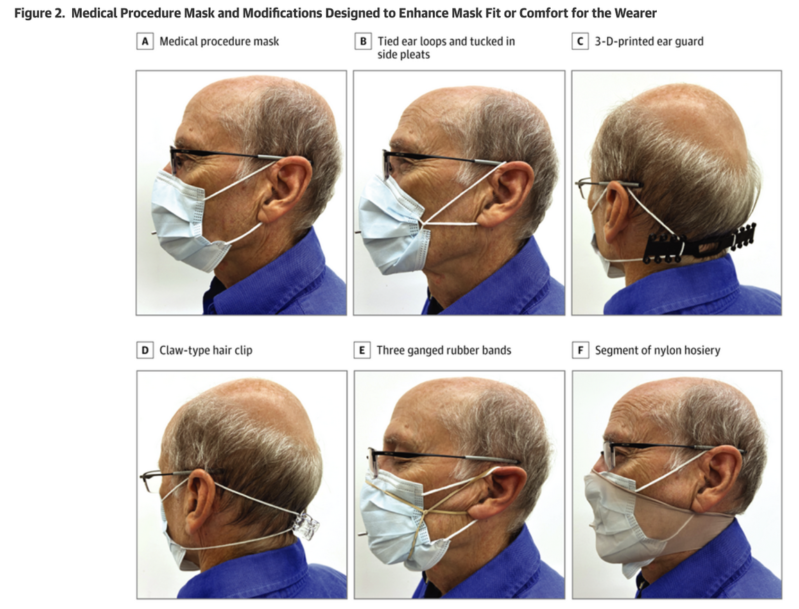
- Limitations include that all masks were tested on a single adult male and that the size of the sodium chloride particles may not represent the typical size of the droplets that carry SARS-CoV-2. Results cannot be used to draw conclusions about mask wearer protection from COVID-19.
Suggested citation: Cash-Goldwasser S, Kardooni S, Cobb L, Bochner A, Bradford E and Shahpar C. In-Depth COVID-19 Science Review December 12 – 18, 2020. Resolve to Save Lives. 2020 December 22. Available from https://preventepidemics.org/covid19/science/review/